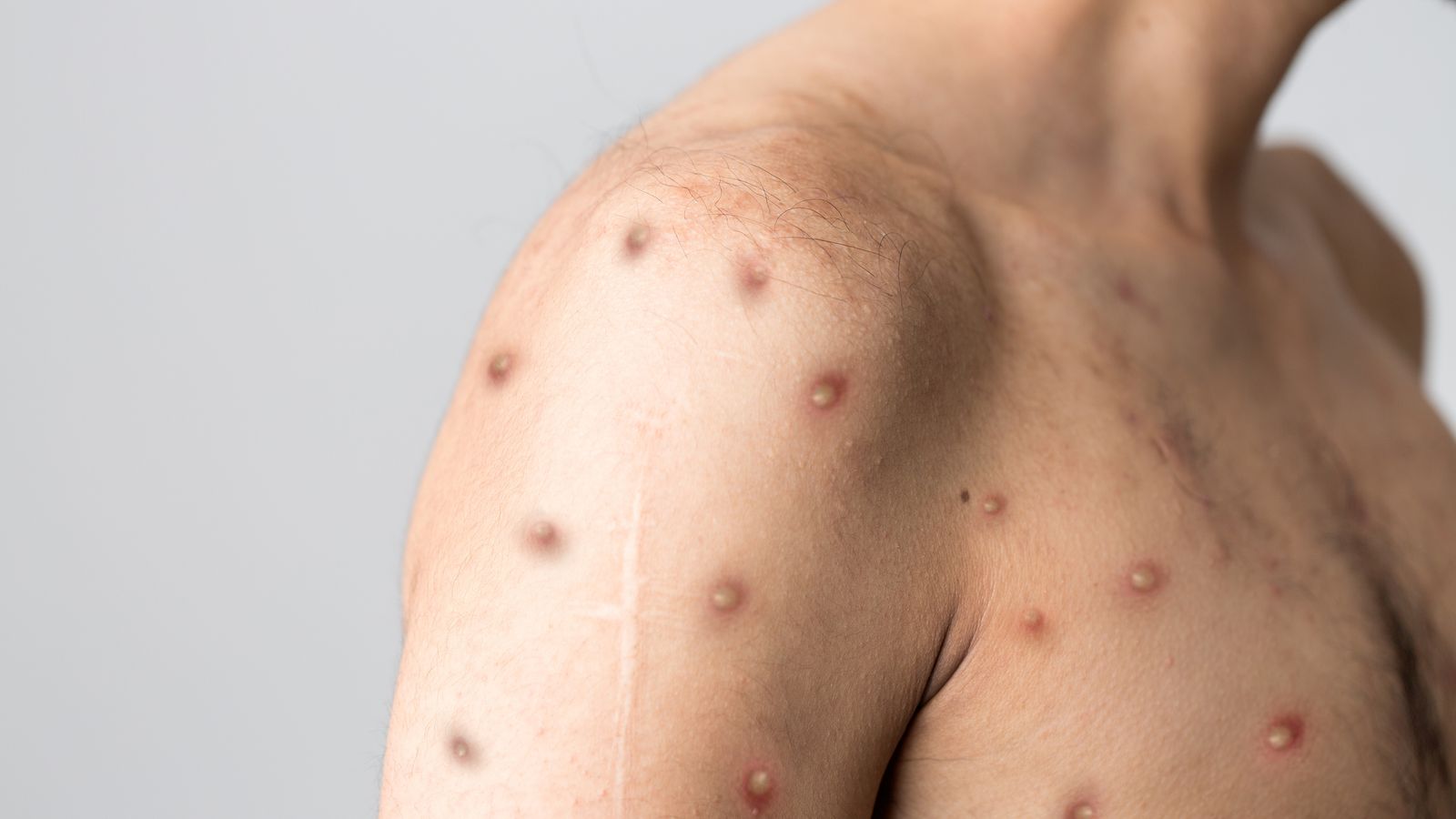
Sexual health providers fear they could be forced to stop seeing vulnerable and at risk patients in some parts of the country unless they receive extra government funding to cover the cost of tackling the Monkeypox outbreak.
In a letter to NHS England, the UK Health Security Agency (UKHSA), and the Department of Health and Social Care, sexual health leaders say on average 25-30% of all services have been replaced by Monkeypox assistance since the first case was identified in early May.
This includes a 90% reduction in access to STI screening in the most affected areas, and half of providers needing to reduce their PrEP delivery services to those at risk of contracting HIV by 25%.
They say this drop in appointments for assessment and treatment has resulted in outbreaks of STIs in several parts of the country.
The letter signed by the British HIV Association, and the British Association for Sexual Health and HIV says: “In some cases this displacement in financial terms means a potential loss of income to clinics of over £600,000 per quarter.
“This level of loss of income risks destabilising clinics, with loss of staff and, as some providers have warned us, the potential exit from the market of some providers.”
Sexual health leaders also say that vaccination funding of £15 per dose delivered has yet to reach any of the clinics, doesn’t meet the cost of providing the service and doesn’t cover providers for work displacement.
Read more:
Monkeypox: How do you catch it, what are the symptoms, and how easily does it spread?
Different strain detected in the UK after patient travelled to West Africa
In a separate letter to Public Health Directors and Commissioning Officers at District Councils, they pleaded for funding to not be withdrawn while they seek extra funding.
“After repeated advocacy with the government and with NHS England/Improvement, we are still at the stage of these national agencies repeatedly requesting evidence while this burden on services remains unfunded,” the letter reads.
“We continue to press them for MPX funding and have repeatedly advised them that the exceptional nature of this epidemic, the transmission routes of MPX and its impact should not be considered as routine sexual health expenditure.”
Responding to the letters, a Department of Health and Social Care spokesperson said: “We continue to work closely with the UK Health Security Agency, local authorities and NHS England to manage pressures on sexual reproductive health services and ensure access to routine services is maintained.
“The Public Health Grant will increase in each of the next three years, bolstering sexual health services and enabling people to access treatments faster.”
Sky News analysis has found spending on sexual health clinics has reduced in almost every local authority in England since the service was passed on to local governments’ responsibility in 2013, according to data from local authority revenue expenditure and financing.
There have been 3,654 confirmed or highly probable cases of Monkeypox since 6 May, at its peak in mid-July there were around 60 cases per day. That number decreased throughout August and continues to fall.
More than 45,000 people have received a dose of the Monkeypox vaccine, including around 40,000 gay, bisexual and other men who have sex with men and who are at highest risk of exposure.
Those at highest risk continue to be prioritised but some clinics will offer second doses to provide longer term protection to vulnerable groups two to three months after they receive the first dose, with the NHS inviting those eligible to come forward.